Psychosocial Issues
Personal Impact of HIV
People with HIV face difficult times—their family and friends included. Washington State provides a resource for infected and affected HIV/AIDS persons that can connect them with the necessary support services they need. A medical case manager is usually the primary contact for help. This medical advisor can provide information about medical care facilities and support programs available, including information about volunteer groups in the area, insurance agencies who specialize in HIV & AIDS, hospice care, and other supportive services. Their goal is to help improve and maintain health for those living with HIV and hopefully bring them a better sense of independence.
A useful source for those looking for a medical case manager is the Washington State HIV Case Management Directory. It can be accessed here:http://www.doh.wa.gov/YouandYourFamily/IllnessandDisease/HIVAIDS/HIVCareClientServices.
Otherwise, information can be obtained by calling Washington State Department of Health at 1-877-376-9316.
Lifelong Challenges & Difficult Realities
Living with HIV/AIDS is a challenging feat. It commands a multitude of difficult decisions and conjures up emotional turbulences that require a lot of strength and support from others. It involves moving forward and doing so courageously and hopefully obtaining new perspectives concerning life, gaining new insights, and moving in new directions. Any type of challenge takes courage from a person, and living with HIV is definitely one that requires fortitude to move ahead. Those living with HIV struggle with negative thoughts, and too, with attitudes and beliefs that are aimed at them from others, which only adds to the stress that is already brought on by the diagnosis of HIV/AIDS.
One of the difficult realities facing people with HIV include their need to adhere to strict medication regimens—else face dire consequences that could mean life or death for them.
Another problem is procuring adequate insurance coverage so prescribed treatments can be obtained as needed.

A large concern, as with any chronic disease, is that most people living with HIV often experience anxiety, depression, or other mental health problems. At some point, they will likely need psychosocial support.
Higher rates of substance abuse, including alcohol and tobacco use, are normally prominent in cases with HIV.
One major alarm to HIV—infected people include the responsibilities they have in protecting their partners from becoming infected. This involves disclosing their HIV status to potential sex or needle—sharing partners and practicing safer sex behaviors.
Issues of stigma and discrimination especially affect HIV men who have sex with men. This pertains highly for injection drug users as well. They are often subjected to social and job—related discrimination, which increases with a diagnosis of HIV or AIDS.
Caregiver Needs
At some point in the life of an HIV/AIDS person, assistance is needed from a caregiver, as with others who experience chronic diseases. Standard precautions are seriously advised for any caregiver in a homecare setting of an HIV patient. Each caregiver should know preparations for a realistic level of risk. Important self—care is recommended as follows:
Basic Guidelines for the Caregiver:
- Set realistic limits to caregiving. Be aware and respect your time and responsibility that goes along with that care.
- Be sure to ask questions of other health care providers when you don’t understand what is needed in a particular setting.
- Concerning employment with a homecare agency, discuss withyour employer ways to perform your job that reduces stress and burn out.
- UNIVERSAL and STANDARD PRECAUTIONS should always be remembered for not only you, but also for the patient's health and welfare.
- As needed, seek support from professionals and peers to maintain your effectiveness and morale as a caregiver.
Special Populations to Consider
HIV infection can affect people from all ethnic groups, genders, ages, and income levels, but some groups tend to be significantly affected by the AIDS epidemic. Such groups include 1) men who have sex with men; 2) injecting drug users; 3) people with hemophilia; 4) women, and; 5) people of color.
Take note of the information that follows concerning the different populations that are affected by the AIDS epidemic. It’s important to be aware in order to provide the necessary support where these cases are concerned.
Men Who Have Sex with Men (MSM)
TThe HIV—infected proportion in Washington State that are men who have sex with men (MSM)—adults and adolescents—is estimated at 69.7% of their population. 8.2% are MSM who also inject drugs, which makes their HIV risk even higher. Reported by CDC, out of the estimated 47,500 Americans that were newly infected with HIV1 in 2010, 26%—about 12,200—were adolescents or young adults aged 13–24 years. It was shown that young men who have sex with men (YMSM), especially black/African Americans YMSM, are at highest risk.
No matter how our society is changing concerning this matter homosexuality, there are still a lot of American societies who have issues and are against it. It’s important to realize and recognize the legal rights of gay and lesbian people, for it is expanding. Yet this does not mean acceptance by all members of society.
As a healthcare worker, it is your responsibility to be aware of the stigma and discrimination factors present with the HIV population as it influences the “experience” of all men who have sex with men (MSM), including those living with HIV. Reluctance to seek HIV testing and medical care can result on the part of MSM due to this knowledge of ill acceptance. They may not receive positive support from some traditional sources, such as churches and civic groups. These groups may be unwilling to give support to gay and lesbian people because of the stigma attached to HIV, AIDS, and homosexuality.

OOther issues relate to low self—esteem and other psychological issues (including depression, anxiety, mental health problems, and risk—taking behaviors) that may cause, or be made worse, due to stigma and discrimination against MSM. Also, constant and annoying messages to HIV—negative men who have sex with men sometimes become fatigued with “safe sex” messages and will focus less of their attention on protecting themselves from HIV infection. Some may even feel that HIV infection is inevitable and engage in unprotected sex.
Another challenge is faced by the MSM who also has sex with women. They may not exclusively identify themselves as "gay" and then it is difficult to reach those men who do not identify as being “gay” with HIV prevention efforts and activities. Lacking the social and community resources they need, some bisexual men tend to face challenges much similar to "gay" men.
A summary of major challenges for MSM & YMSM include:
- Limited awareness of infection
- Low perception of risk
- Inadequate HIV prevention education and intervention
- Alcohol and illegal drug use
- Feelings of rejection and isolation
Drug Users
One of the most vulnerable groups to HIV infection are those who inject drugs (also known as PWID). The prevalence to HIV for these people is said to be 28 times higher than among the rest of the population. On average, one in ten new HIV infections are caused by the sharing of needles. Globally, this accounts for almost a third of HIV infections outside of sub—Saharan Africa (where HIV is most prevalent).
According to AVERT, a pioneer in providing HIV and AIDS information since the start of the epidemic, it is estimated that there are 12 million people who inject drugs worldwide, and around 1.6 million (one in seven) who are thought to be living with HIV. China, Russia and the United States account for nearly half of all people who inject drugs globally.
Washington State’s 2015 State Health Profile relates that 5.5% of their HIV diagnosed cases were from drug injection transmission (last estimation calculated in 2013).
Because drug use is often criminalized and stigmatized, PWID is among those who have the least access to HIV prevention, treatment and healthcare. The UN goal of halving new HIV infections among injection users was only reduced by 10% in 2015. Another issue that relates to the lack of help concerning this category of HIV risks, societies tend to look down on those with illegal drug use and individuals who come from poverty—stricken and homeless environments and sometimes view them as “deserving” their infection.
Prevention programs have been created that assists in reducing the harmful effects from poor injection practices. One such program is the syringe exchange program where injection users are provided clean needles in exchange for their used ones. This provision encourages safe use practice and has proven to reduce the transmission of blood—borne pathogens like HIV, HBV, and HCV. However, such programs are controversial, as some people believe that this service can actually instigate and give messages of “approval" for their injection drug use. Though not proven by evidence, it certainly constitutes the possibility.
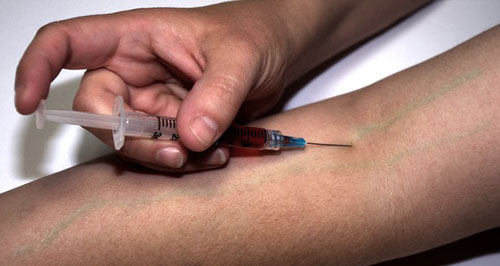
As with any individual who feels degraded or lessened by how the public views them, issues of poverty, self—esteem, and psychological matters are prevalent with injection drug users. They suffer depression, anxiety, and mental illnesses and are apt to involve themselves in risk—taking behaviors. These complications only multiply their problems, inciting their addiction, and making it more difficult for them to stop.
Treatment facilities are few; demand is large. This poses yet another problem for those who would like treatment and help in correcting their addition. Many of these people are placed on waiting lists, and the time it takes to place them, make the follow—up more difficult and sometimes lost. The possibly of poor and dysfunctional living may have them moving to different locations, or simply the wait has encouraged enhanced addiction habits and lessened the “help me” factor.
Hemophiliacs
In a condition called Hemophilia (sometimes spelled Haemophilia), blood is unable to clot properly, which then causes excessive bleeding (external and internal) after any injury or damage. This inherited bleeding disorder is estimated by CDC to affect 1 in 5,000 male births. About 400 babies are born with hemophilia each year. Though it affects females as well, it is shown to be more prevalent in males.
Characterized by lower than normal—clotting factors circulating in the blood, treatment for hemophilia includes the use of products like "factor VIII" and "factor IX" which are clotting material pooled out of donated blood plasma. Without such treatment, hemophiliacs could bleed to death.
Receiving these concentrates, however, the hemophiliac has to obtain injections of the clotting factors that they lack, which in turn allows them to lead relatively normal lives. Raw materials for these concentrates come from donated blood, meaning that prior to the advent blood testing, many hemophiliacs were infected with HIV.
Unfortunately, ninety percent of severe hemophiliacs contracted HIV and/or HCV in the 1980s through the use of these products. Anger arose at that time as there was evidence showing that the company’s manufacturing of these concentrates knew of the possibility of their products being contaminated, yet they distributed them anyway.
Though some people considered these hemophiliacs to be "innocent victims" of HIV, nonetheless they received significant discrimination. Two noteworthy cases resulted in The Ricky Ray Relief Fund Act and the Ryan White Care Act—named after two HIV—positive hemophiliacs.
The Ricky Ray incident involved three brothers—Ricky, Robert and Randy—all born with hemophilia and diagnosed with HIV as children. In 1986, they were not allowed to attend school following their positive test results. A court ruled the following year that they had every legal right to attend, but their family's home was burned to the ground the week following the decision.
The Ryan White case was another who rallied for his right to attend school. These two programs continue to act as HIV/AIDS support programs.
Women with HIV
According to the CDC, women represent 20% of the estimated 1.2 million cumulative AIDS diagnoses in the United States from the beginning of the epidemic through the end of 2014. About one fifth constitutes for new infections each year, most of which are attributed to heterosexual sex. Another common transmission is due to drug injection use by their partners. Women of color have shown to have higher risks.
Factors that increase the risk of HIV infection in women:
- During unprotected vaginal sex, HIV passes more easily from a man to a woman than from a woman to a man.
- Age—related thinning and dryness of the vagina increase the risk of HIV infection due to skin breakages in the vaginal wall.
- A woman’s partner is more likely to be involved in high—risk behaviors, such as injection drug use or having unprotected sex with other men.
Many of the issues concerning HIV—infected women from partners include those who assumed their relationship to be monogamous, only to find out there were other sexual partners. Some are unable to discuss or implement safer sex practices due to issues of self—efficacy and/or domestic violence affecting their relationship.
A woman will most likely postpone taking medication or going to medical appointments due to having to care for their children or other family members.
Other issues involve fear of disclosing their HIV status to others. They fear losing their jobs, housing, or experience other forms of fear that are linked to discrimination. Single parents with HIV may feel particularly fearful because of their lack of support.
Lack of transportation, lack of health insurance, limited education and low income are common problems that keep HIV infected women from receiving appropriate treatment. Child—care problems tend to prevent them from going to medical appointments.
Women will often feel they have more pressing problems or concerns and place their HIV infection second as their symptoms may present as being mild and manageable for years. Lack of income, housing expense, no access to medical care, being in abusive relationships, and having children to take care of are just some of the ongoing topics involving women with HIV.
People of Color
Higher instances of HIV/AIDS appear in African Americans and Hispanics, despite that there are no biological reasons for the disparities. Although African American and Hispanic women make up less than 25% of the total U.S. population, 77% account for all reported AIDS cases in women. Half of new HIV cases in the U.S. are African American, even though they make up only 12% of the population. 20% of AIDS cases in the United States are Hispanics, yet Hispanics make up 13% of the population.
There is no single reason as to why these differences exist. One factor seems to be linked to socioeconomic conditions. Another factor may deal with distrust of the healthcare system. It has been shown that many people of color do not trust the system for a variety of reasons. Access to early intervention and treatment has found to be due to a number of reasons. Adequate housing, food, and employment are among some of the major problems existing among people of color.
Diversity is a main factor among these populations. Immigrant status, religion, languages, geographic locations and, as stated before, socioeconomic conditions, get in the way and cause challenging situations.
Denial about HIV risk, stigmatization, and discrimination all play parts in how these people relate to their disease. Religious institutions or respected "elders" in the community may help, even though, ironically, these institutions or elders are some of the very ones who contributed to the misinformation and stigma associated with HIV.
For HIV Prevention Programs to be effective, they have to recognize the need of working with diverse communities and realize the importance of planning, evaluating HIV activities, and delivering appropriate messages culturally and linguistically.